An intrauterine device, commonly known as an IUD, is a small, ‘T’-shaped piece of equipment that is gently inserted into the uterus. This device is a powerful player in the world of long-term contraception, offering a highly effective, reversible solution for those seeking extensive protection against pregnancy.
The beauty of an IUD lies in its simplicity and longevity. Once it’s in place, it requires minimal maintenance and can provide anywhere from 3 to 10 years of contraceptive coverage, depending on the type. This makes it an excellent choice for those who desire a “set it and forget it” approach to birth control.
IUDs come in two main types: hormonal and copper. The hormonal IUD releases a small amount of progestin, a hormone that thickens the cervical mucus to prevent sperm from reaching the egg. The copper Intrauterine device, on the other hand, releases copper ions, which are toxic to sperm.
What makes particularly appealing is its reversibility. If you decide that you’re ready to start a family or if you want to switch to a different form of contraception, your healthcare provider can easily remove the Intrauterine device. Following removal, fertility typically returns to normal fairly quickly.
Types of IUD available:
1. Copper IUD
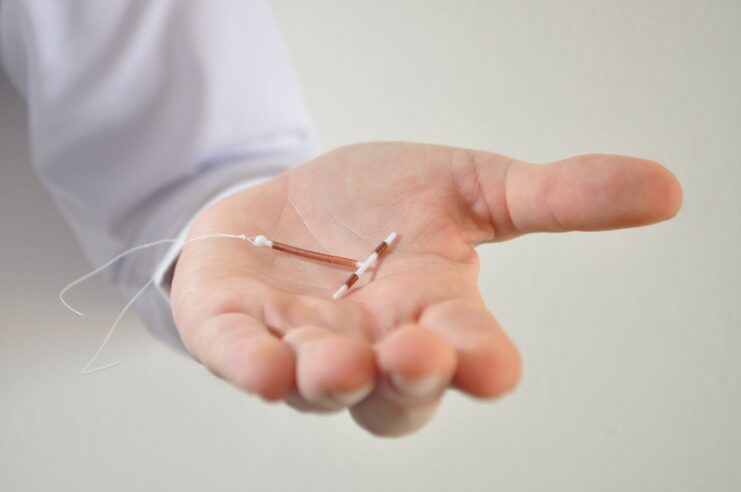
The copper IUD is able to provide long term contraception for up to 5 years. It works by damaging sperms so that fertilization is disrupted. Copper also acts as a spermicide within the uterus, disrupting the motility and viability of sperms.
Besides acting as a form of long term contraception, the copper Intrauterine device can also be used as a form of emergency contraception (EC) and is the most effective form of EC available (better than the hormonal EC pills). The copper can be used as an EC up to 5 days after unprotected sex.
2. Hormonal
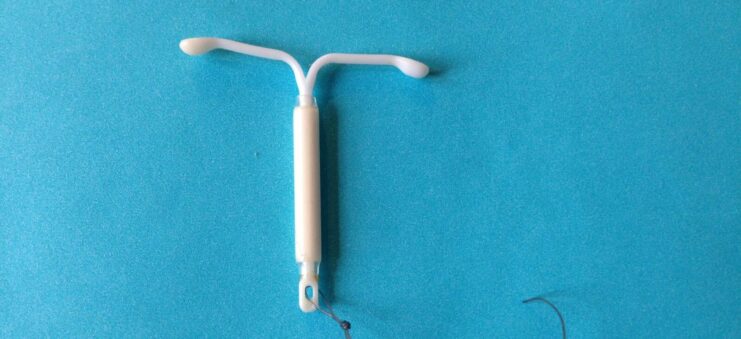
Hormonal IUDs such as Mirena contain the hormone levonorgestrel which acts by releasing small amount of hormone regularly. This thickens the cervical mucus and while thinning the endometrial lining, making it unfavourable for fertilization and implantation to occur.
As the hormone levonorgestrel causes thinning of the endometrial lining, the Mirena can be used to treat women who experience heavy bleeding (menorrhagia). In the majority of women, bleeding becomes lighter or stops within 6 months after insertion.
Benefits
- There is no need to take daily contraceptive pills.
- Most effective form of long term contraception.
- Cost-effective. Though the initial cost of fitting the IUD cost more, the fact that most Intrauterine devices can be used for more than 3 years makes them cheaper than other forms of contraception over the same period of time.
- Quick return of fertility upon removal.
- Can be inserted immediately after delivery or termination of pregnancy.
- Safe in women who are breastfeeding.
Side Effects and Risks
Like any medical intervention, IUDs come with potential side effects and risks. For instance, hormonal IUDs may cause irregular bleeding, headaches, breast tenderness, and mood changes, especially in the first few months after insertion.
Copper Intrauterine devices may lead to heavier periods and more cramping. There’s also a small risk of the Intrauterine device being expelled from the uterus or, in rare cases, perforating the uterine wall. It’s important to discuss these potential risks and side effects with a healthcare provider.
Who Can Use IUDs:
While they are suitable for many people, they’re not the best choice for everyone. For example, individuals with certain health conditions, such as breast cancer or liver disease, may not be able to use hormonal ones. Copper IUDs may not be suitable for those with copper allergy or Wilson’s disease.
Women with active pelvic infections or certain uterine abnormalities may not be able to use Intrauterine devices at all. A healthcare provider can help determine if an IUD is a good choice based on individual health history and lifestyle factors.
The Process Insertion and Removal:

Understanding what to expect during Intrauterine device insertion and removal can help alleviate any anxiety. Both procedures are usually quick and can be done in a healthcare provider’s office.
Insertion involves placing the IUD into the uterus through the cervix, which may cause some discomfort or cramping. Removal involves a healthcare provider gently pulling on the Intrauterine device’s strings, which hang down into the vagina. Some women may experience light bleeding after sex or cramping after removal.
Epilogue
In conclusion, an intrauterine device (IUD) offers a highly effective, long-term, and reversible method of contraception that can be tailored to individual needs and lifestyles. Whether you choose a copper Intrauterine device or a hormonal IUD, this small, ‘T’-shaped device provides extensive protection against pregnancy with minimal maintenance.
The benefits of Intrauterine devices are numerous, from their cost-effectiveness over time to their quick return of fertility upon removal. However, like any medical intervention, they come with potential side effects and risks, which should be discussed with a healthcare provider.












