Molluscum Contagiosum is a common skin condition that often raises concerns due to its appearance. However, understanding its nature, causes, and treatments can help alleviate worries. In this comprehensive guide, we’ll delve deep into this condition, breaking down its complexities for everyone to grasp.
Molluscum Contagiosum is a viral skin infection that results in round, firm, painless bumps ranging in size. While it’s most commonly found in children, adults can also be affected, especially those with weakened immune systems.
What is Molluscum Contagiosum?
Molluscum Contagiosum, often just referred to as molluscum, is caused by the molluscum contagiosum virus (MCV). This virus is part of the poxvirus family and is known for the distinctive bumps it causes on the skin. These bumps are typically small, shiny, and can be pink, white, or skin-colored.
The condition is generally harmless and tends to resolve on its own. However, it’s contagious and can spread to other parts of the body or to other people through direct contact or shared objects.
History and Prevalence
Historically, Molluscum Contagiosum has been a known skin condition for centuries. Its name is derived from Latin, where “molluscus” means soft. The condition is prevalent worldwide, with children, people living in tropical climates, and those with compromised immune systems being the most affected.
In recent years, there has been a rise in cases, especially in urban areas. This could be attributed to increased close physical contact activities and shared use of facilities.
Symptoms and Identification
Recognizing the symptoms of Molluscum Contagiosum is the first step towards managing the condition. The primary symptom is the appearance of small, raised bumps on the skin.
Appearance of the Bumps
- Color: The bumps are usually pink, white, or skin-colored.
- Shape: They are round and dome-shaped, often with a dimple in the center.
- Size: Typically, they range from 2 to 5 millimeters in diameter.
- Texture: They are smooth and firm to touch.
The bumps can appear anywhere on the body but are commonly found on the face, neck, armpits, arms, and hands in children. In adults, they are often found on the genitals, abdomen, and inner thighs.
Associated Symptoms
While the bumps are generally painless, they can become itchy or sore, especially if they become inflamed or infected. Scratching them can lead to secondary bacterial infections. In some cases, redness or swelling might be observed around the bump.
Causes and Transmission
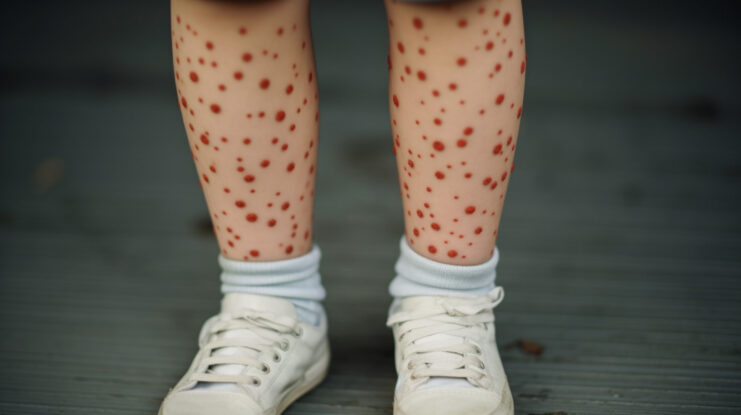
Understanding how Molluscum Contagiosum spreads can help in its prevention and management.
How it Spreads
Molluscum Contagiosum is highly contagious. It can spread through:
- Direct skin-to-skin contact: This is the most common mode of transmission.
- Contact with contaminated objects: Towels, clothing, toys, or any other object that has been in contact with an infected person’s bumps can transmit the virus.
- Scratching or touching the bumps: This can transfer the virus to other parts of the body.
Risk Factors
Certain groups of people are more susceptible to contracting the virus:
- Children: Especially those between the ages of 1 and 10.
- People with weakened immune systems: This includes individuals with HIV/AIDS or those undergoing chemotherapy.
- Individuals with atopic dermatitis: Their broken skin barrier makes them more vulnerable.
Treatment Options
Navigating through the various treatment options can be overwhelming. However, understanding the available methods can help in making an informed decision.
When is Treatment Necessary?
While Molluscum Contagiosum often resolves on its own, there are situations where treatment might be considered:
- Cosmetic concerns: Some individuals might want the bumps removed with surgery for aesthetic reasons.
- Discomfort: If the bumps are itchy or painful.
- Risk of spreading: To prevent passing the condition to others.
Common Treatment Methods
- Cryotherapy: This involves freezing the bumps using liquid nitrogen.
- Curettage: The bumps are scraped off using a curette.
- Laser therapy: High-intensity light is used to destroy the bumps.
- Topical treatments: Creams or ointments, such as those containing salicylic acid or imiquimod, are applied to the bumps.
It’s essential to consult with a dermatologist to determine the best treatment option for your specific situation.
Prevention and Care

Preventing the spread of Molluscum Contagiosum is crucial, especially if you or someone close to you has been diagnosed.
Preventive Measures
- Avoid direct skin contact with someone who has the condition.
- Do not share personal items, such as towels, clothing, or toys, with an infected person.
- Keep the bumps covered with clothing or a bandage.
- Refrain from scratching or picking at the bumps.
Aftercare Tips
- Moisturize regularly to prevent skin dryness and reduce itching.
- Avoid swimming in public pools until the condition has cleared to prevent spreading.
- Wash hands frequently to reduce the risk of spreading the virus to other parts of the body.
Impact on Daily Life

Living with Molluscum Contagiosum can have both physical and emotional impacts.
Physical Implications
While the condition itself is not painful, the bumps can become itchy or sore, especially if they are in areas with frequent friction, like the inner thighs.
While many skin conditions like Molluscum Contagiosum are benign, it’s essential to be aware of more serious conditions, such as skin cancers, which can arise from factors like prolonged sun exposure.
FAQs
Is Molluscum Contagiosum dangerous?
No, Molluscum Contagiosum is generally a benign condition. While the bumps might be unsightly or cause discomfort, they are not dangerous. However, secondary infections can arise if the bumps are scratched or picked at.
How long does it last?
In most cases, the bumps caused by Molluscum Contagiosum will clear up on their own within 6 to 12 months. However, in some individuals, especially those with weakened immune systems, the condition can last longer.
Conclusion
Molluscum Contagiosum, while common, is often misunderstood. Recognizing its symptoms and understanding its causes can help in its effective management. It’s essential to remember that while the condition is contagious, it’s generally harmless and resolves on its own. If you or someone you know is affected, it’s always a good idea to consult a dermatologist for guidance.