In the realm of skin conditions, keloids and hypertrophic scars stand out as some of the most intriguing yet misunderstood phenomena. These scars, often seen as unsightly blemishes, are a testament to the body’s incredible ability to heal, albeit sometimes in an exaggerated manner.
This article delves deep into the world of these unique scars, shedding light on their causes, characteristics, and the myriad of treatment options available.
What are they?
Keloids scars/ hypertrophic scars are a very common lesion. Practically everyone in Singapore knows or has seen someone with an unusually large firm fleshy (or sometimes red) lesion over the left deltoid region (the so-called BCG scar).
Keloid
Keloids and hypertrophic scars are formed by the body’s exaggerated healing response to wounds and injuries. When you get a cut or a wound the body will heal itself by closing the defect with fibrous tissue. This can sometimes leave a small mark known as a scar. Occasionally, the healing process may be exaggerated and you get an abnormally large or prominent scar, otherwise known as a keloid or a hypertrophic scar.
There are other skin variations like Fordyce spots on the vulva, which are harmless but can cause concern due to their unfamiliar appearance.
Hypertrophic scars can be distinguished from keloids by the following:
Hypertrophic scar
- Hypertrophic scars tend to stay to the margin of the original wound
- They generally tend to soften and flatten over time, unlike keloids, which progress to grow over the years.
Why do I get them?
As previously stated, these lesions tend to develop after injuries to the skin. Keloids and hypertrophic scars can arise from anything, from surgical scars, ear piercings, BCG vaccinations to even trivial causes such as acne. There is no hard and fast rule to predict who or even which skin lesion will develop into a hypertrophic scar or a keloid.
The areas over the sternum (upper chest), deltoid (shoulder) and the upper back tend to have an increased risk of keloid and hypertrophic scar formation.
Keloids and hypertrophic scars are also noted to be associated with infected wounds, foreign bodies in the wound, wounds with high tension closure and repeated trauma. Additionally, keloids tends to form more frequently in Asians and darker-skinned people.
Are they dangerous?
Neither keloids nor hypertrophic scars are dangerous. They may however cause localized irritation, itching and occasionally pain. If either forms in an area of the skin exposed to frequent motion, this may cause friction and discomfort. Keloid scars in particular are quite unsightly and many people are keen to get rid of them for this reason.
What should I do?
The best way to treat keloids and hypertrophic scars is to not let them occur in the first place. This means taking care of any wounds, keeping them clean and avoiding contamination. Appropriate and timely closure of large wounds such as cuts and lacerations may also reduce the risk of keloid and hypertrophic scar formation. There are a number of topical applications available that are targeted to minimize poor wound healing. However, even with your best efforts, it may not be possible to prevent them from happening.
How do I get rid of it?
Both hypertrophic and keloid scars can be treated in similar ways, although keloid scars tend to respond less favourably and have a higher chance of recurrence. In addition, hypertrophic scars tend to flatten and soften over time, unlike keloid scars which usually get bigger with time.
Classically, intralesional steroid injections have been used to treat keloids and hypertrophic scars, with a good degree of success.
Intralesional steroid injection
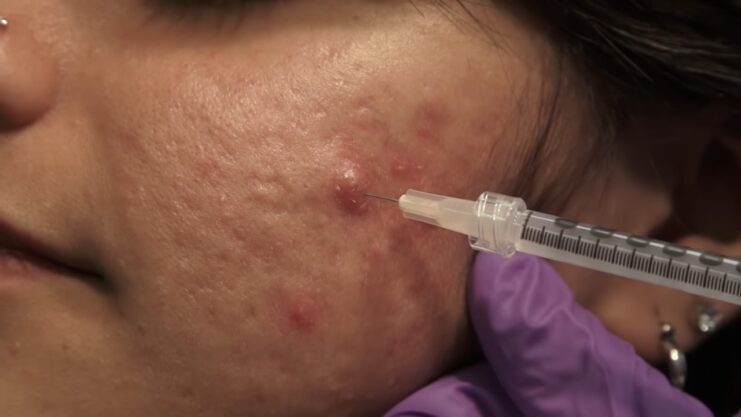
While it may flatten the lesion, the discoloration or atrophic appearance of the scar will often remain. Steroid injections must also be applied cautiously for fear of thinning the skin. For this reason, the course of treatment is usually a series of injections applied to the lesion over the duration of a few weeks or even months, rather than a single large depot dose of steroid.
There are a lot of topical applications in the market that are available to help reduce keloids and hypertrophic scars. These applications often include retinoic acids, Vitamins A and E, corticosteroids as well as antihistamines. Response to these creams has been varying.
Compression of the lesions also seems to help, particularly with keloid wounds. Its thought to interfere with the continued inflammatory process associated with the progressive growth of keloids. However, compression often needs to be applied for up to 23 hours daily for 6 months of more. This makes it impracticable for facial and other visible keloid lesions.
Cryotherapy has recently been used with good respone. The cyro-agent is used to induce cellular destruction in the keloid or hypertrophic scar over a series of sessions.While it shows good results in up to 60% of lesions, it is important to note that cryotherapy may cause hypopigmentation.
Surgical excision is usually a last resort when it comes to dealing with keloids in particular. There is always a chance that the keloid will recur or even worsen post surgery. Hypertrophic scar tend to respond a bit better.
Recently, there have been combinations of traditional surgical excision with laser irradiation and external beam therapy to prevent the reactive regeneration of the lesion. However this has to be used very cautiously, as there is a potential for beam radiation to potentiate tumors.
Final Words
Keloids and hypertrophic scars, while not dangerous, can be a source of discomfort and self-consciousness for many. Understanding their nature and the available treatments is the first step towards managing and potentially reducing their appearance.
Remember, every scar tells a story, and while we might seek to diminish its prominence, it’s a testament to our body’s resilience and ability to heal.












