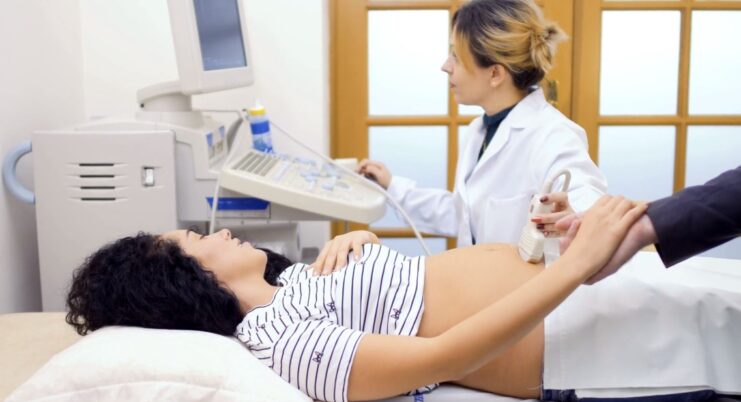
Ultrasound technology has revolutionized the medical field in numerous ways. One of its significant applications is in the realm of fertility assessment. For many, the journey to parenthood can be fraught with challenges, and understanding the role of ultrasound can provide clarity and hope.
In this article, we delve deep into the uses of ultrasound in fertility assessment, aiming to provide valuable insights for those embarking on this journey.
Ultrasound, a non-invasive imaging technique, has become an indispensable tool in the realm of reproductive medicine. Its ability to provide real-time images of the internal structures of the body has made it a go-to method for many fertility specialists.
Basic Imaging Assessment
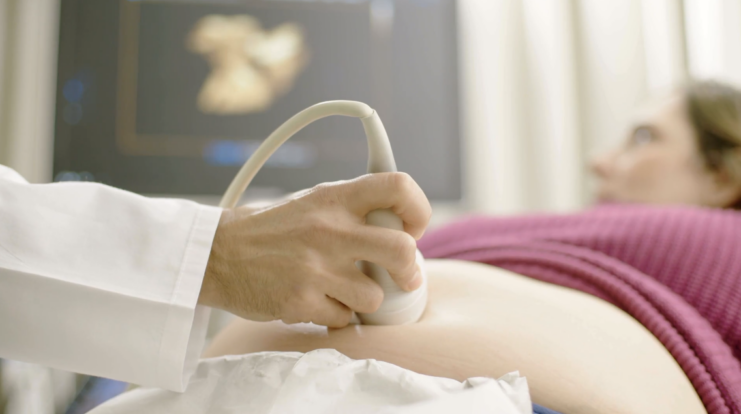
The simple answer to whether ultrasound can be used during fertility assessment is a resounding yes. As a foundational step, ultrasound serves as a basic imaging assessment to screen for abnormalities of the female reproductive organs.
A transvaginal ultrasound, in particular, offers a clear visualization of the cervix, uterus, endometrium (uterus lining), and ovaries. Detecting anatomical variants like a bicornuate uterus or physical abnormalities such as fibroids early on can pave the way for more specialized interventions.
Differentiating Follicles from Cysts
When examining the ovaries, specialists assess their size, shape, and the number of follicles present. The number of follicles can vary depending on the menstrual cycle phase, necessitating two scans approximately six weeks apart.
This differentiation is crucial because follicles, which are normal, can resemble cysts, which might be abnormal but usually aren’t serious. A consistent appearance between scans indicates cysts, while variations suggest follicles.
- On the left: Ovarian follicles.
- On the right: Cysts.
The similarities can be striking, emphasizing the importance of assessing at different cycle points.
Polycystic Ovary Syndrome (PCOS) and Ultrasound
PCOS is a prevalent condition that can hinder fertility in women. Its root cause is a hormonal imbalance, leading to issues like irregular periods, which in turn complicates pinpointing ovulation times.
Diagnosing PCOS
Ultrasound proves invaluable in diagnosing PCOS. On an ultrasound scan, PCOS manifests as 12 or more identifiable cysts situated at the ovary’s periphery, creating a ‘string of pearls’ appearance.
- Visual Representation: Almost like a string of pearls, albeit with a bit of imagination!
Treatment Implications
Once diagnosed with PCOS, the next step involves deciding on a treatment plan. The hormonal imbalances associated with PCOS can disrupt the endometrium’s maintenance, even if fertilization occurs. This disruption can result in a menstrual cycle as if no implantation took place, leading to potential frustrations for those trying to conceive.
Serial Ultrasounds: Tracking Ovulation
Understanding ovulation is pivotal for fertility. Serial ultrasounds, conducted over several days around the ovulatory period, can identify the dominant follicle set to release the ovum or egg.
Identifying the Dominant Follicle
As ovulation nears, typically one follicle, either in the right or left ovary, enlarges as it matures. Regular ultrasounds during this phase can pinpoint this dominant follicle. Post-ovulation, this follicle transforms into the corpus luteum, responsible for hormone production to sustain the endometrium and facilitate embryo implantation.
The Ring of Fire: Signifying Ovulation
On an ultrasound, the corpus luteum exhibits a distinct “ring of fire” appearance due to its highly vascular outer ring, essential for hormone production and release. Recognizing the corpus luteum indicates ovulation, marking the most fertile period, approximately 72 hours.
Early Pregnancy and Ultrasound
The journey of fertility doesn’t end with conception. Once successful implantation occurs, the next exciting phase begins early pregnancy. Ultrasound continues to play a pivotal role during this period, offering glimpses into the developing life within.
The First Glimpse
The first few weeks of pregnancy are filled with anticipation. Around 6-8 weeks into the pregnancy, an ultrasound can provide the first visual confirmation of the baby. This scan can reveal the baby’s heartbeat, a rhythmic flutter that brings joy to many expectant parents.
This early scan not only confirms the pregnancy but also ensures that the embryo is developing in the right place, ruling out conditions like ectopic pregnancies.
Monitoring Growth and Development
As the weeks progress, the embryo undergoes rapid changes, transitioning into a fetus. Regular ultrasounds help monitor these developments, ensuring that growth is on track. Specialists can measure various parameters, such as the crown-rump length, to estimate the gestational age and predict the due date.
Ultrasound Beyond Fertility
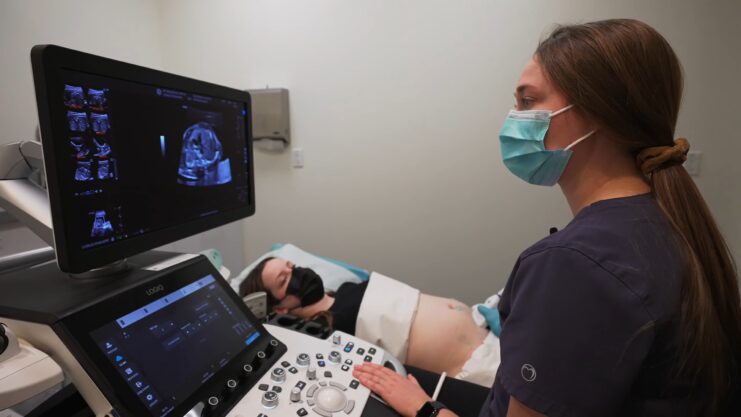
While the primary focus of this article is on fertility, it’s worth noting that ultrasound’s applications extend beyond conception and early pregnancy.
Gender Reveal and Anatomical Scan
Around the mid-pregnancy mark, usually between 18-22 weeks, a detailed anatomical scan is performed. This scan assesses the baby’s organs and structures, ensuring everything is developing as it should. For many parents, this scan also offers the thrilling opportunity to learn the baby’s gender, if they choose to find out.
Third Trimester Scans
As the pregnancy progresses into the third trimester, ultrasounds can monitor the baby’s position, estimate fetal weight, and check the placenta’s location and health. These scans ensure that both mother and baby are ready for the upcoming birth, identifying any potential complications that might necessitate medical intervention.
The Safety of Ultrasound
Given its frequent use during fertility assessment and pregnancy, it’s natural to wonder about ultrasound’s safety.
Non-Invasive and Radiation-Free
One of the primary benefits of ultrasound is its non-invasive nature. Unlike X-rays, ultrasounds don’t use ionizing radiation, making them safe for both mother and baby. Instead, they utilize sound waves to create images of the internal structures.
Decades of Safe Use
Ultrasound technology has been in use for several decades, with countless studies affirming its safety. While it’s always essential to use medical interventions judiciously, ultrasounds, when used appropriately by trained professionals, pose minimal risks.
FAQ
1. How long does a fertility ultrasound take?
Typically, a fertility ultrasound takes about 20-30 minutes. However, the duration might vary based on the specific details being assessed.
2. Is the ultrasound procedure painful?
While the transvaginal ultrasound might cause slight discomfort, it’s generally not painful. If you experience any pain, it’s essential to communicate with the technician.
3. How often should I get ultrasounds during fertility treatments?
The frequency of ultrasounds during fertility treatments depends on the specific treatment plan and individual needs. It’s best to consult with your fertility specialist for personalized advice.
4. Can ultrasounds detect male fertility issues?
While ultrasounds are primarily used for female fertility assessments, they can also be used to detect certain male fertility issues, such as varicoceles or obstructions in the ejaculatory ducts.
5. Are there any side effects after undergoing a fertility ultrasound?
Ultrasounds are generally safe and non-invasive. Most individuals experience no side effects. However, some might feel slight tenderness or discomfort, which usually subsides quickly.
Wrapping Up
In wrapping up, the journey of fertility and early pregnancy is a profound experience, filled with anticipation, hope, and sometimes challenges. Ultrasound stands as a beacon of light during this journey, offering insights, assurance, and the joy of seeing life unfold.
Whether you’re at the start of your fertility journey or awaiting the arrival of your little one, embrace the marvels of modern medicine and the wonders it brings.
Related Posts:
- Missed Periods – a Sign of Fertility as Well as Infertility
- Vaginal Bleeding During Early Pregnancy: Causes and…
- Sex During Menstruation – The Good, the Bad and the Ugly
- When to Test for HIV During and After Completion of…
- Foods To Avoid During Pregnancy: Nourishing Your Baby Bum
- Understanding Vulvovaginal Candidiasis: The Itch You…